TMS THERAPY
FDA-cleared, non-medication depression treatment
For those diagnosed with depression, specific areas of the brain are known to be underactive. Stimulating these areas can improve the brain’s ability to regulate mood.
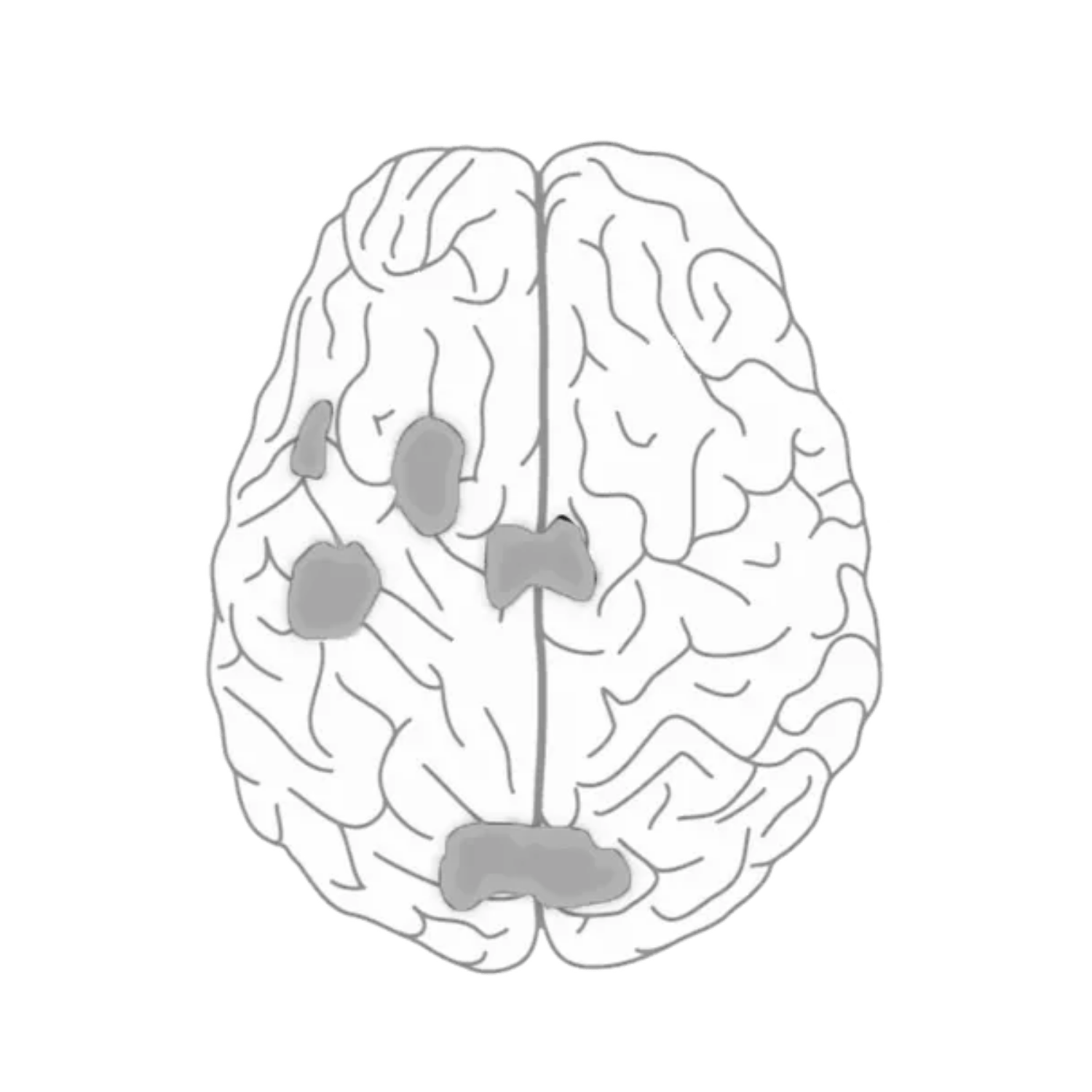
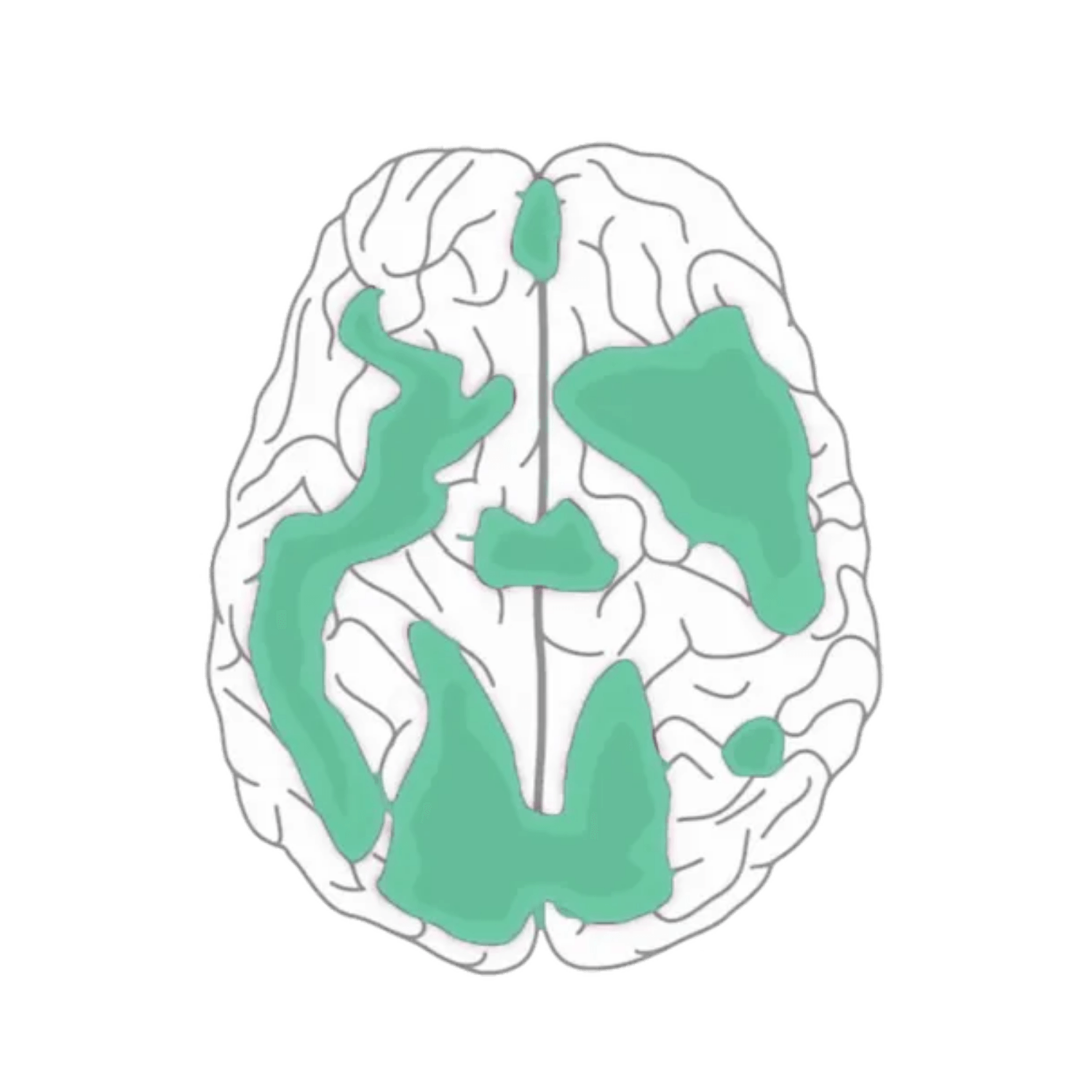
Source: Mark George, M.D. Biological Psychiatry Branch Division of Intramural Research Programs, NIMH 1993.
INNOVATIVE TREATMENT SOLUTIONS
FDA-cleared since 2008
Antidepressants have worked to treat depression for many people since the 1980s, but they don't work for everyone. TMS therapy isn’t an antidepressant medication. Instead, it works by using gentle magnetic pulses.
Targeted to you
Unlike medications, which affect the entire body as they pass through the blood-brain barrier, TMS therapy targets depression at the source. That means you don’t have to put up with drug-related side effects, such as gastrointestinal problems, trouble sleeping, or weight gain.
Go right back to your day
Unlike other forms of brain stimulation, TMS therapy is non-invasive and non-sedating. Treatment sessions take place in our private centers and you can drive yourself to and from treatment. You can go back to work or school right away.
Dedicated to you
Your Care Team – providers, patient consultants, TMS technicians – are here for you. We work with you every step of the way to ensure that you're getting the care you need.
FDA-cleared since 2008
Since the 1980s, treatment for depression has consisted mostly of antidepressants. Lots of people have felt better from antidepressants, but they don’t work for everyone. TMS therapy isn’t an antidepressant medication. Instead, it works by using gentle magnetic pulses.
Targeted to you
Unlike medications, which affect the entire body as they pass through the blood-brain barrier, TMS therapy targets depression at the source. That means you don’t have to put up with drug-related side effects, such as gastrointestinal problems, trouble sleeping, or weight gain.
Go right back to your day
Unlike other forms of brain stimulation, TMS therapy is non-invasive and non-sedating. Treatment sessions take place in our private centers and you can drive yourself to and from treatment. You can go back to work or school right away.
Dedicated to you
Your Care Team – providers, patient consultants, TMS technicians – are here for you. We work with you every step of the way to ensure you're getting the care you need. Your TMS Technician will be with you during treatments and you're free to chat with them or just sit and relax.
Proven success
Like : Talk therapy & Antidepressants
Many of our patients have had tried multiple treatment methods before finding success with TMS.
Other applications
TMS therapy is indicated for multiple conditions, with more research being done every day
safe, effective, and comfortable
TMS has far fewer side effects compared to antidepressant medications. With more than 10,000 treatments performed in clinical trials, the most common side effect was mild-moderate scalp discomfort.
If you have symptoms of depression, it’s natural to wonder how TMS is different from medications and talk
therapy. Medications aren’t as customizable
— they may not work for genetic reasons and
could cause moderate to severe side effects.
Symptoms of depression can also interfere with the comfort and effectiveness of talk therapy.
TMS targets the area of the brain that is believed to regulate mood to treat depression at its neurological source.er what’s going on in your body. The good news is that researchers have now answered two crucial questions: how does depression affect the brain, and what chemical imbalance causes depression? These discoveries can help you on your journey toward recovery.
https://www.greenbrooktms.com/blog/how-does-depression-affect-the-brain/
https://www.youtube.com/watch?v=nwMKNn6g_g0&list=PLfBiZcu2B1ag-fOtr9fieH2lSlRmSbCyA&index=4
If you've been dealing with treatment-resistant depression, you've likely already tried several depression medications or therapies. Maybe they only partially worked, or didn't work at all, so now you're considering transcranial magnetic stimulation, or TMS. At this point, all you want is to find relief, so you're probably wondering how long before TMS works. Read on to learn more about TMS and when you might feel better if you try it.
https://www.youtube.com/watch?v=gM9BOfvvQMs&list=PLfBiZcu2B1ag-fOtr9fieH2lSlRmSbCyA&index=2
Searching for the right depression treatment can be frustrating. It's not always a matter of taking a pill and seeing your symptoms go away—everyone's experience with antidepressants is a little different.
Non-drug and FDA-cleared
Non-invasive with no drug-related side effects.
Covered by most insurance
We handle the paperwork.
Fits into your existing treatment
Can be stand-alone treatment or along with your existing medication.
Zero downtime
Drive yourself to and from treatments. Get back to your day right away, including work or school.
The most important question
Non-drug and FDA-cleared
Non-invasive with no drug-related side effects.
Covered by most insurance
We handle the paperwork.
Fits into your existing treatment
Can be stand-alone treatment or along with your existing medication.
Zero downtime
Drive yourself to and from treatments. Get back to your day right away, including work or school.
Greenbrook TMS supports an accessible internet. If you have any questions about our accessibility features, please contact us at
866.928.6076 and/or info@greenbrooktms.com.
All Rights Reserved | Greenbrook TMS NeuroHealth Centers.